HOW TO PREVENT Degenerative Joint Disease ESPECIALLY HIP REPLACEMENT. EASY! A FEW TRICKS.
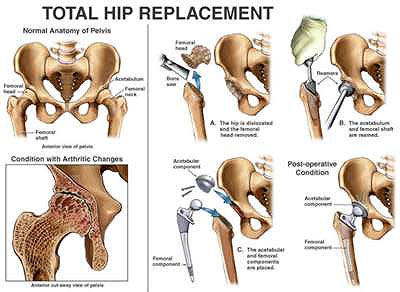
NOTHING is MORE GENETICALLY PASSED ON than the tendency to get those creaky, painful, swollen HIP BONES, the ones that have to be replaced with steel in what used to be the longest operation that exists, l0 plus hours, so that the anesthesia halved your IQ but now I hear it's an hour and a bit. I worry as I can feel my own joint wearing out early, pain if I walk crooked. It is a totally genetic thing. A suceptability! I have the bad hip, My dad had it, my Aunt had it, My brother had it. Replacements of that socket bone required for them, not me yet at 77 yrs but thank SCIENCE it's no longer like those earlier surgeries -- ten HOURS of SURGERY. Not nowadays according to my brother; it's down to two hours.But the CO-PAY? OUCH! That hurts the nearest thing to the hip, the WALLET! Well, luckily, we're shown by a great holistic DOCTOR how to prevent degenerating hip bones. If your hips are melting, save this file for your grandkids as THEY WILL HAVE this weakness. Tendency to have eroded bones is genetic. PREVENTION of it is everything. Glucosamine Chondroitan is recommended, below.
http://drbenkim.com/prevent-osteoporosis.html
http://www.drbenkim.com/how-to-stretch-inner-hip.htm
Another doctor writes: Definition of Degenerative Joint Disease
A degeneration or ‘wear and tear’ of articular (joint surface) cartilage is usually accompanied by an overgrowth of bone (osteophytes), narrowing of the joint space, sclerosis or hardening of bone at the joint surface, and deformity in joints. OA is not usually associated with inflammation, although swelling of the joint does frequently occur in OA. This type of arthritis is called osteoarthritis, OA, degenerative joint disease, DJD, or osteoarthrosis. Other forms of arthritis (rheumatoid, post-traumatic, and other inflammatory disorders) frequently may have OA as the end-stage, making differentiation difficult.
Description of Degenerative Joint Disease
The tissues involved most in osteoarthritis are the cartilage and underlying subchondral bone. The cartilage is the smooth white material that forms over the ends of the bones and forms the moving surface of the joint on both sides. Cartilage is tough, elastic, very durable, and comprised of collagen and water molecules. Cartilage does not have a blood supply and receives its oxygen and nutrition from the surrounding joint fluid by diffusion. The ability of cartilage to absorb nutrients and fluid allows it to function without a blood supply.
When we move a joint, the pressure across the joint expresses fluid and waste products out of the cartilage cells, and when the pressure is relieved, the fluid diffuses back, together with oxygen and nutrients. Hence the health of the cartilage depends on movement of the joint.
Over many years and with activity and use of a joint, the cartilage may become frayed, injured, torn, and may even wear away entirely. When this occurs, the bone surface on one side of the joint tends to rub or glide against the bone on the opposite side of the joint, providing a less elastic joint surface, and generating higher contact pressures at the end of the bone. Over time, the contacting bone surfaces become hardened and ‘sclerotic’, a process that causes the bone to look polished and on x-rays produces a whitened appearance.
There are three common forms of osteoarthritis, and many people have some of each type. All people will develop OA to some degree, involving one or more joints, throughout their lifetime as the aging process advances. The most common sites for OA include the base of the thumb joint, the knees, and the hands.
The first and mildest form causes bony enlargement of the finger joints. The end joints of the fingers become bony (this is due to osteophyte formation, or reactive bone at the joint surfaces) and the hand begins to assume the appearance we associate with old age – i.e., a swollen joint involving the fingers. The base of the thumb may become swollen with bony enlargement and is the most frequently encountered site of OA.
The second form involves the spine (neck and mid- and low-back regions). Bony growths (osteophytes) appear on the spine in the neck region or in the lower back. Usually the bony growths are associated with some narrowing of the space between the vertebrae. Similar to the long-bone cartilage joint space degeneration, the process of OA in the spine begins with a degeneration of the cartilage in the disc spaces. These disc spaces degenerate, narrow, and lead to increased forces on the bones, with subsequent osteophyte formation.
The third form involves the weight-bearing joints,most frequently involving the knees, which are followed by the hips.
The symptoms of OA may become quite severe. Osteoarthritis of the weight-bearing joints, particularly the hip and knee, develops slowly and often (but not always) involves both sides of the body. Pain in the joint may remain fairly constant or may wax and wane for a period of years, and usually is activity related. In advanced cases, walking or regular activities of daily living may become difficult or even impossible. Reactive fluid (an effusion) may accumulate in the affected joint, giving it a swollen appearance. This fluid is generated from the soft tissue in the knee known as synovium, which reacts by trying to create more lubrication to make the joint surfaces smoother. A knee may feel unsteady, stiff, or have a sensation of giving out when weight is placed on it. Additionally, a feeling of locking or grinding may be felt in the joint.
Usually, in the knee, the osteoarthritis will affect the inner half of the joint more than the outer. This may result in progressive deformity with the leg becoming bowed and may cause difficulty in walking. OA involving the outer half of the knee may cause a “knock-knee” appearance. Generally, this form and deformity of arthritis is less common, and it is more often associated with other forms of arthritis, such as rheumatoid arthritis.
Causes and Risk Factors of Degenerative Joint Disease
Osteoarthritis is the most common form of joint disease, sparing no age, race, or geographic area. At least 20 million adults in the U.S. suffer from osteoarthritis. Symptomatic disease increases with age. Many patients may have OA seen on x-rays, but not be overly symptomatic.
Hereditary, injury, fractures around a joint surface, and overuse factors are most frequently involved in the development of osteoarthritis. Osteoarthritis may occur secondary to an injury to the joint due to a fracture, repetitive or overuse injury, or metabolic disorders (e.g., hyperparathyroidism). Additionally, gout and other forms of crystalline joint disease may lead to OA of a joint. Obesity or being overweight is a risk factor for knee osteoarthritis more commonly in females; this is less commonly seen in the hip joint. Recreational running does not increase the incidence of OA, but participation in competitive contact sports does. Specifically, impact sports that repetitively load a joint increase the injury to a joint. If cartilage in a joint is injured, it cannot regenerate, and the new forces that are created are abnormal, leading to further stresses, and the cycle may propagate.
Symptoms of Degenerative Joint Disease
Initially there may be joint stiffness, usually lasting more than 15 minutes, and typically following activity of the joint. Later there may be pain on motion of the affected joint, which is made worse with activity or weight-bearing and relieved by rest. Typically OA improves with rest and does not remain symptomatic at night time. It is usually better in the morning, and it worsens as the day progresses.There may be limitation of motion of the affected joint, although this is a later finding. Coarse crepitus (a creaking or cracking) may be felt in the joint. There is usually some mild joint swelling and tenderness to touch. The joint may feel warm. A joint that cracks and snaps does not necessarily mean arthritis is present, and many patients are able to make their joints crack without having pain.
Diagnosis of Degenerative Joint Disease
Diagnosis is based on the medical history, physical examination, and x-ray findings. Lab tests do not reveal signs of inflammation, but may be performed to rule out other arthritic disorders.Treatment of Degenerative Joint Disease
Treatment of OA depends upon multiple factors including patient age, activities, medical condition, and x-ray findings. Patients with mild to moderate osteoarthritis of weight-bearing joints (hips and knees) may benefit from a supervised exercise program such as walking. Non-impact activities such as swimming, cycling, and walking tend to be more comfortable for patients with OA. In a younger patient with signs or symptoms of OA, other causes of arthritis such as deformity, medical conditions, or bone disorders should be carefully sought for in order to rule out other conditions.A program of regular physical activity can strengthen the muscles, tendons, and ligaments surrounding the affected joints and preserve mobility in joints that are developing bone spurs. Many physicians believe that osteoarthritis may be prevented by good health habits. Remaining active, maintaining an ideal body weight, and exercising the muscles and joints regularly so as to nourish cartilage.
A first line of simple treatment - acetaminophen (Tylenol) is as effective and has less side effects than other non-steroidal anti-inflammatory drugs (NSAIDS) such as ibuprofen, naproxen, or aspirin.
Glucosamine-chondroitin sulfate may be prescribed by your doctor. This medication, when taken over a period of months, may reduce pain and symptoms by restoring or replenishing nutrition to diseased cartilage cells. It tends to be more effective in earlier stages of OA. The dosage and combination of each ingredient is an important aspect of the therapy, as not all preparations and brands are the same. Patients who fail to improve on acetaminophen or glucosamine may be treated with salicylates and other oral anti-inflammatories ( NSAIDs). Previously, medications such as Vioxx, Celebrex, and Bextra (Cox-2 NSAIDS) were preferred due to less gastrointestinal side effects (ulcers) and improved pain relief for arthritis. However, currently the use of these medications should be reviewed with your doctor, as concerns about their use in certain patients has been recently reported. More traditional NSAIDS (ibuprofen, naproxen, etc.) are available over the counter, and they also provide excellent relief of symptoms. Capsaicin cream 0.25% applied twice daily may reduce knee pain. Intra-articular (within the joint) injections of steroids may also be helpful, although the duration and amount of pain relief is often unpredictable, especially in more advanced stages of OA. Alternative injections of hyaluronic acid peparations (sodium hyaluronate) are also available and may be very useful in the treatment of OA. These injections are indicated for OA of the knee, and typically require an injection once a week, over a period of three to five weeks (i.e., three to five injections). The hyaluronic acid is injected into the knee joint, and similar to oral glucosamine, may provide nutrition to the diseased cartilage cells and collagen within the cartilage. The fluid is a gel-like material that appears to act initially like a lubricant for the joint. However, studies have shown that the lubricant aspect plays little role and, in fact, the fluid is absorbed quickly by the cartilage cells.
Bracing, splinting, and other orthotic treatments may be useful in managing or “unloading” an arthritic joint surface. These nonoperative treatments are simple, often effective, however cost and ease of use are factors in their selection in treatment.
Surgery may be dramatically effective for patients with severe osteoarthritis of the weight-bearing joints. Total hip replacement and newer hip resurfacing replacements and total knee replacement or unicompartmental (partial) knee replacement can be extremely effective. Joint replacement is now being performed in younger patients also. The concerns about wear of the prosthetic joint surface in younger patients make this the most challenging aspect of future research in this area. Newer joint surfaces for joint replacement including highly cross-linked polyethylene, metal on metal bearing, ceramic bearings, and others have emerged and currently are available in the U.S.
Although arthroscopic surgery for knee osteoarthritis is a common procedure, its long-term effectiveness is unclear, and may be best for symptoms such as catching, locking, or those that have been present for only a short duration. In addition, not all patients that have arthritis should have an arthroscopy, as this may not improve their symptoms.
In younger patients, hip and knee preserving procedures should be considered, in order to avoid a hip or knee replacement. Although performed less frequently, hip and knee preserving procedures, such as osteotomy (cutting the bone and realigning the bone or joint surface), may restore a joint to a normal alignment and be an excellent alternative to joint replacement.
AlternativeDegenerative Joint Disease
Experimental techniques to repair cartilage loss in the knee by transplantation of cartilage cells is promising. This is most effective in small, localized areas of cartilage loss and not in advanced arthritis. These procedures also may be combined with joint osteotomy to alter joint alignment in order to allow this new cartilage to heal.Prevention of Degenerative Joint Disease
Weight reduction may reduce the risk of symptomatic knee osteoarthritis and, more importantly, reduce the symptoms of OA in the knee in overweigh patients.If you have an injury to your joint, activity modification while maintaining an active lifestyle and joint range of motion provide for a healthy joint recovery.
An actual patient, this poster's brother said: " My doctors uses the newest hip surgery methods. He makes a small incision close to the hip bone. With that small opening, he gains access to the "target" area. The opening was four or five inches long. I'm guessing that he goes in with a power tool to expose hte hip, cut the degnerated bone out, drill a hole and connect the parts. I don't remember any pain. Through some bit of magic, he inserts a 7-inch metallic hip bone. Then, he closes the area with sutures. Several hours after the surgery (which takes only one to two hours), the nurse awakens me to have me walk a few steps. I must keep the leg fairly straight. Next day is the same routine. I am forced to walk a few steps. Approximately three days later, I am transported via ambulance (cost over $1000) for a few blocks to a convalescent home. I stay there for seven days. Then, I am released to go home. Within another seven days, I am able to walk without a cane or walker. Finally, after another seven days, I can run slowly. So, in a period less than a month, the leg has healed, and I am ready to have surgery on my second leg."
I was back in my bed at a relatively early time. Ten hours may have been the amount of time back in the 20th century, but we have moved ahead. I'ts two now.
I consider my surgeon an absolute genius. As I recall, three days in the hospital, one week in the convalescent place (with a very noisy neighbor), then home.
Article updated and reviewed by Stephen Burnett, MD, FRCS(C), Assistant Professor, Department of Orthopaedic Surgery, Washington University School of Medicine on July 11, 2005.
Questions To Ask Your Doctor About Degenerative Joint Disease
Are there clinical signs of degenerative joint disease (based upon history and examination)?
If I am a younger patient, should I be evaluated for another cause, other than OA, that may be surgically correctable?
Are x-rays indicated?
Are other tests, such as blood work and MRI indicated?
Would exercise or activity change help?
Is there a role for bracing, orthotics, or other splints?
What medications do you recommend – analgesics, anti-inflammatories, glucosamine?
Should I consider an injection, and, if so, what type: steroid versus hyaluronic acid?
What are the side-effects of any of these medications or injections?
Will surgery be required, and is there a non-joint replacement option/alternative?
What can be done to retard the degenerative process? QUIT TEA. It is highly diuretic, passes the urine out to the ocean with your bones in it.
Pain is a symtom, ergo LUCKY FOR YOU as it will you you that you have a problem, however it can be confusing because there are many causes. It is important to make an accurate diagnosis of the cause of your symptoms so that appropriate treatment can be directed at the underlying problem. If you have hip pain, some common causes include:
Arthritis is among the most frequent causes of hip pain, and there are many treatments available. If conservative treatments fail, hip replacement surgery is an option.
Trochanteric bursitis is an extremely common problem that causes inflammation of the bursa over the outside of the hip joint.
Tendonitis can occur in any of the tendons that surround the hip joint. The most frequently encountered tendonitis around the hip is iliotibial band (IT band) tendonitis. Yoga on hip area works to get the cause of tendonitis GONE. Uric acid deposits.
* Osteonecrosis
Osteonecrosis is a condition that occurs when blood flow to an area of bone is restricted. If an inadequate amount of blood flow reaches the bone, the cells will die and the bone may collapse. One of the most common places for osteonecrosis to occur is in the hip joint. So do deep crouches regularly to get circulation into the joint.
* Lumbar Pain - Referred Symptoms
Many back and spine problems can cause symptoms around the buttocks and hip. The most common problems that refer pain to the hip region are herniated discs and sciatica.* Snapping Hip Syndrome
Snapping hip syndrome is a word used to describe three distinct hip problems. The first is when the IT band snaps over the outside of the thigh. The second occurs when the deep hip flexor snaps over the front of the hip joint. Finally, tears of the cartilage, or labrum, around the hip socket can cause a snapping sensation.* Muscle Strains
Strains of the muscles around the hip and pelvis can cause pain and spasm. The most common strains are groin pulls and hamstring strains.* Hip Fracture
Hip fractures are most common in elderly patients with osteoporosis. Treatment of broken hips requires surgery to either replace the broken portion or repair it with a metal plate and screws.* Stress Fracture
Stress fractures of the hip are most common in athletes who participate in high-impact sports, such as long distance runners. Treatment usually is successful by avoiding the impact activities.Childhood Hip Problems:
* Developmental Dysplasia
When the hips are dislocated or out of position in infancy, the joint may not develop properly. While this is not usually painful as a child, it will lead to early arthritis and problems with walking. Certain dog breeds get this.* Legg-Calve-Perthes Disease
Also called Perthes disease, this is a problem similar to osteonecrosis (see above) but in childhood. If severe, it can lead to permanent damage to this hip joint and early arthritis.When do you need to call your doctor about your hip pain?
If you are unsure of the cause of your symptoms, or if you do not know the specific treatment recommendations for your condition, you should seek medical attention. Treatment of hip pain must be directed at the specific cause of your problem. Some signs that you should be seen by a doctor include:o Inability to walk comfortably on the affected side
o Injury that causes deformity around the joint
o Hip pain that occurs at night or while resting
o Hip pain that persists beyond a few days
o Inability to bend the hip
o Swelling of the hip or the thigh area
o Signs of an infection, including fever, redness, warmth
o Any other unusual symptomsWhat are the best treatments for hip pain? http://orthopedics.about.com/cs/hipsurgery/a/hippain.htm
Treatment depends entirely on the cause of the problem. Therefore, it is of utmost importance that you understand the cause of your symptoms before embarking on a treatment program. If you are unsure of your diagnosis, or the severity of your condition, you should seek medical advice before beginning any treatment plan.
Some common treatments for hip pain are listed here. Not all of these treatments are appropriate for every condition, but they may be helpful in your situation.
* Rest: The first treatment for most conditions that cause hip pain is to rest the joint, and allow the acute inflammation to subside. Often this is the only step needed to relieve hip pain. If the symptoms are severe, crutches or a cane may be helpful as well.
* Ice and Heat Application: Ice packs and heat pads are among the most commonly used treatments for inflammation. So which one is the right one to use, ice or heat? And how long should the ice or heat treatments last? Read on for more information about ice and heat treatment.
* Stretching YOGA: Stretching the muscles and tendons that surround the joint can help with some causes of hip pain. A good routine should be established, and following some specific suggestions will help you on your way. Yoga is deep breathing INTO the painful stretch.
* Physical Therapy: Physical therapy is an important aspect of treatment of almost all orthopedic conditions. Physical therapists use different modalities to increase strength, regain mobility, and help return patients to their pre-injury level of activity. Get deep tissue massage on the area.
* Anti-Inflammatory Medication: Nonsteroidal anti-inflammatory medications, commonly referred to as NSAIDs, are some of the most frequently prescribed medications, especially for patients with hip pain caused by problems such as arthritis, bursitis, and tendonitis. But it's a phony cure unless you deep tissue massage the cream IN, a half hour of work dedicated to creating circulation.
* * * * * * * * * * * * * * * * * * * * * * * * *
Our POSTER is ANITA SANDS HERNANDEZ, Los Angeles Writer, Futurist and Astrologer. Catch up with her websites TRUTHS GOV WILL HIDE & NEVER TELL YOU, also The FUTURE, WHAT'S COMIN' AT YA! FRUGAL LIFE STYLE TIPS, HOW TO SURVIVE the COMING GREAT DEPRESSION, and Secrets of Nature, HOLISTIC, AFFORDABLE HEALING. Also ARTISANRY FOR EXPORT, EARN EUROS....* Anita is at astrology@earthlink.net ). Get a 35$ natal horoscope "my money/future life" reading now + copy horoscope as a Gif file graphic! No smarter, more accurate career reading out there!
<=== BACK TO TRACKING THE ECONOMY, an INDEX PAGE
<===BACK TO MONEY SECRETS ONLY THE EXPERTS KNOW
<=== BACK TO SECRETS THE GOV DOES NOT WANT YOU TO KNOW
<===BACK TO THE SECRETS OF THE OLIGARCHS, THE EMPIRE INDEX PAGE
<=== SHOW ME THE FIX INDEX PAGE.
<== SHOW ME THE HAPPY R)EVOLUTION PAGE
<=== BACK TO "GUERILLA CAPITALISM" -- THE SOLUTION!
<==== BACK TO THE "VITAL SIGNS OF A DYING ECONOMY" the "FUTURE" WEBPAGE
<==== BACK TO THE WALL STREET MELTDOWN WEBSITE, with "WHAT TO DO TO SURVIVE" TIPS
<=== BACK TO ENRON PLANET, the DOOMSDAY SCENARIO!
<====BACK TO THE HOLISTIC GOURMET, BON MARCHE
<=== BACK TO THE GLEENERS PAGE
<=== BACK TO THE FRUGAL INDEX PAGE
<== BACK TO THE FUTURE -- WHAT'S COMIN' AT YA! AN INDEX PAGE
<=== BACK TO THE GENTLEMAN FARMER'S GARDEN INDEX
<=== INVESTIGATE DOING DRIP IRRIGATE- LINES in DROUGHT GARDENS for BIG $, Learn in 1 hr at Home Depot
<=== BACK TO THE ACTIVISM IS A DELIGHT PAGE
<=== BACK TO THE MALTHUSIAN INDEX PAGE
<===BACK TO THE PHILOSOPHY INDEX PAGE
<=== BACK TO THE LUCK IN LOVE WEBSITE
<== BACK TO THE PROPAGANDA STUDIES WEBSITE, HOW GOV LIES TO YOU
<=== BACK TO ALL POINTS OF THE COMPASS POLITICAL PHILOSOPHY TUTORIAL
<=== BACK TO JERRY'S REFRIGERATOR & the Tin Foil Hat Collection of CONSPIRACY THEORIES!
<=== BACK TO THE GLOBAL ELITE AND THE DAMAGE THEY DO
<===BACK TO THE HISTORY OF EMPIRES AND EMPERORS
<===BACK TO THE "GET TO KNOW YOUR LOCAL OLIGARCH " WEBSITE
<--- BACK TO THE NEWS STORIES YOU WON'T READ IN REGULAR PAPERS WEBPAGE
<=== BACK TO THE HEROES OF ACTIVISM WEBPAGE
<=== EVICTION DANGERS and SOLUTIONS
<=== BACK TO THE HARD TIMES INDEX PAGE
<== BACK TO THE CREATE A CHARITY & SALARY YOURSELF WEBPAGE
<==BACK TO THE HOLISTIC ARCHIVE, 100 WAYS TO REJUVENATE, PREVENT DISEASE
<===BACK TO THE REAL ESTATE INDEX SO POOR PEOPLE CAN BUY
<==== BACK TO HOW TO REALLY CLEAN A HOUSE
<==== PORTAL to 7,000 ARTICLES, REPUBLISH FREE, ATTRACT HUGE AD REVENUE TO YOUR BLOG